|
 |
 |
| Barbara Stewart-Knox | Syka Iqbal | Muhammad Waqas |
Researchers from the University of Bradford explore the relationship between food bank access and better mental health, highlighting the implications of their work for the United Nations’ Sustainable Development Goals.
We became interested in food security and mental health in the wake of the sharp economic downturn post Covid-19, alongside unprecedented geopolitical events that led to rising energy and food.
In the United Kingdom (UK), this was characterised by an increase in household spending on food and decreased outside the home.
Our previous work using Understanding Society data showed that these changes in food spending were associated with poorer mental health. In particular, rising food expenditure was linked to worse mental health in lower income households, adding to the growing list of challenges already faced by disadvantaged groups.
This finding highlighted widening health inequalities, where already stretched people were living in less affluent circumstances and were more likely to experience declining mental health, alongside having to spend more on food.
A surprising finding arising from our previous work was that individuals on lower incomes with lower food expenditure reported better mental health. In trying to explain this finding, we wondered if they had better mental health and spent less because they were receiving food aid.
We then began to wonder if food bank usage, which according to The Trussel Trust has increased by 120% over the past five years, could help to explain population mental health.
Understanding how mental health relates to food aid is important given its implications for the UK to achieve the United Nations (UN) Sustainable Development Goals (SDGs) of irradicating poverty and hunger, reducing inequality and improving mental health by 2030.
How did we use the Understanding Society database?
To explore this further, we analysed data from the Understanding Society survey, which is a large UK panel survey that collects information from around 50,000 individuals in each wave.
Determining the direction of cause-and-effect relationship between mental health and access to food banks, would ideally require a controlled trial. To control food aid as part of a trial would not be ethical with potential for harm to those in the control group who were denied access.
In light of this constraint and given the large size and representativeness of the data base, we were able to use Propensity Score Matching (PSM).
PSM allowed us to create a control group post hoc who were matched on a range of relevant socio-economic and demographic factors and which in comparison to the food bank users, could enable us to gain some insight into whether attending a food bank is beneficial or detrimental to mental health.
We already knew that the Understanding Society database assessed mental health on a rolling yearly basis but had to delve deeper to discover that people were also asked if they accessed a food bank.
Needless to say, we were very pleased to find that the survey not only asked about food bank usage, but also if people had sought but failed to access a food bank.
From this, we were able to derive a further matched sample of those who had sought but were unable to access a food bank and with which to compare mental health with food bank users and with those who had never sought or accessed a food bank.
A database of the size and representativeness of the Understanding Society survey was needed to obtain enough individuals matched on a wide range of socio-economic and demographic factors such as income and to create these groups with which to compare food bank users.
Why propensity matching?
In researching a sensitive topic like mental health and food bank usage, PSM allows control and matching of characteristics in a way similar to that achieved by means of a trial, but without potential for harm to those in need.
The Understanding Society survey was deemed suitable for this type of analysis, given the inclusion of the well-validated General Health Questionnaire (GHQ) used to assess mental health.
The large and diverse sample provided sufficient cases who had accessed food banks and a wide enough range of socio-economic variables including gender, income, education, marital status, number of children, employment status, and government office region.
This enabled us to derive a closely matched sample of people who had sought and failed to access assistance through a food bank in addition to those who had never sought access to a food bank.
What did we find?
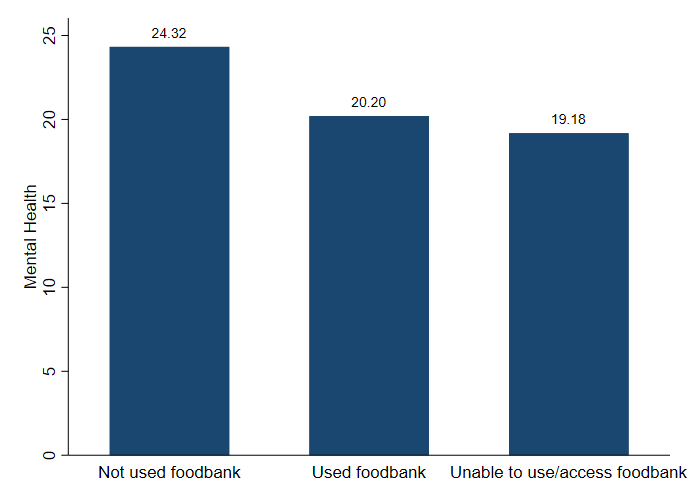
Figure 1 compares mental health between the three groups and clearly shows the inequality between them. It also compares them with the average mental health stated above their respective bar.
We can see that those who had never used a food bank experienced better mental health than those who has accessed or failed to access a food bank.
Figure 1: mental health and food bank usage
Figure 1: The Understanding Society survey assessed mental health using the GHQ for which responses for 12 statements were on a 4-point scale (0 to 3). Scale scores were summed producing a range of 0-36 and then reverse-scored so that higher scores represented better mental health. Larger image / Accessible version.
Given existing research highlighting social stigma around food bank use and the growing controversy around the nutritional quality of food supplied through food banks, we fully expected to find lower mental health among food bank users.
We did not expect to find that access to food banks was associated with better mental health, given current published research highlighting the stigma associated with food aid and the implication that this could impact negatively upon mental health.
Instead, we found evidence to suggest that food banks may provide benefits beyond food provision.
It is not possible, based on these data alone, to determine the mechanisms through which attending a food bank can benefit mental health.
The degree to which food banks impact positively upon mental health could come down to the financial safety net they provide or a response to the interactions with the people working within the food banks and the community social hub that food banks provide.
This is a question we can further probe through qualitative research.
What can we conclude?
Policies are urgently needed to make it easier for more people to access food banks, and to assist food banks to not only provide food but also provide services and support that can improve mental health.
Our findings also highlight the importance of cross-sector collaboration in understanding the interplay between mental health and economic development policies. There are also implications for achieving the United Nations SDGs relevant to reducing inequality and ensuring access to healthy sustainable food.
These challenges are interconnected and can be deeply entrenched and achieving these SDGs will require coordinated action across sectors.
Nonetheless, policies and initiatives directed toward helping households, particularly for low-income households to access food banks, may help bring about a concurrent improvement in mental health alongside addressing food insecurity.
Further research is needed to unpick and better understand the relationships we have identified between food bank usage and mental health. Whatever the mechanism, it is safe to assume that food banks are about much more than food distribution.
You can find out more about our research in our recent paper: A study of mental‐health and food bank use in the UK using propensity score matching.
Meet the authors
Barbara Stewart-Knox is currently an Emeritus Professor of Psychology (food behaviour) at the University of Bradford in West Yorkshire. Barbara also holds an honorary chair in Psychology at Charles Darwin University in Australia.
As an interdisciplinary psychologist, Barbara enjoys collaborative research that addresses the complex dynamics determining food behaviour.
Her research interests are concerned with understanding food choice applied to the promotion of healthy eating, personalised nutrition, food sustainability, inequalities and food product development. This entails the study of psychological wellbeing, attitudinal, perceptual and sensory determinants of food choice and nutrient/food mediated psychological functions.
Syka Iqbal is an Assistant Professor in Psychology at the University of Bradford and an Honorary Research Fellow at the Rapid Research and Appraisal Lab at UCL.
As a health psychologist and behavioural scientist, Syka’s work focuses on the intersections of mental health, prevention science and health inequalities. She has a particular interest in culturally informed and community-engaged approaches, working closely with community organisations, NHS partners and stakeholders to improve outcomes for underrepresented populations.
Her research interests include mental health inequalities, food insecurity and mental health, culturally adapted interventions to inform policy and practice.
Muhammad Waqas is an Assistant Professor at the University of Bradford. Previously, he has worked at the University of Leeds, University of York, University of Sheffield, and the University of Newcastle upon Tyne.
Muhammad has published in prestigious 4* and 3* peer-reviewed journals. He has won research grants as a Principal Investigator from various prestigious funding bodies such as UKRI/ESRC. He has also contributed as a Co-Investigator to various national and multinational, research grant bids.
Muhammad is especially interested in the economics of migration, mental health, subjective well-being, and employing advanced econometrics techniques on interdisciplinary research questions in the field of Psychology, Sociology and Economics.
Comment or question about this blog post?
Please email us!